Manitoba experiencing drought conditions due to warm weather, lack of precipitation
Much of Manitoba is experiencing drought conditions, according to a new report from the Government of Canada.
The report says these dry conditions are due to warm temperatures and a lack of precipitation last month. It notes monthly mean temperatures were well above normal and that much of southern Manitoba recorded less than 40 per cent of normal February precipitation.
The government reports that these weather conditions have caused the expansion of severe drought conditions in an area in south central, and have created an exceptional drought southeast of Brandon and southwest of Portage la Prairie.
According to the report, snowpacks in southern Manitoba are well below normal. Stream flow is near normal on major waterways in the south; however, there are a few reservoirs that are well below normal.
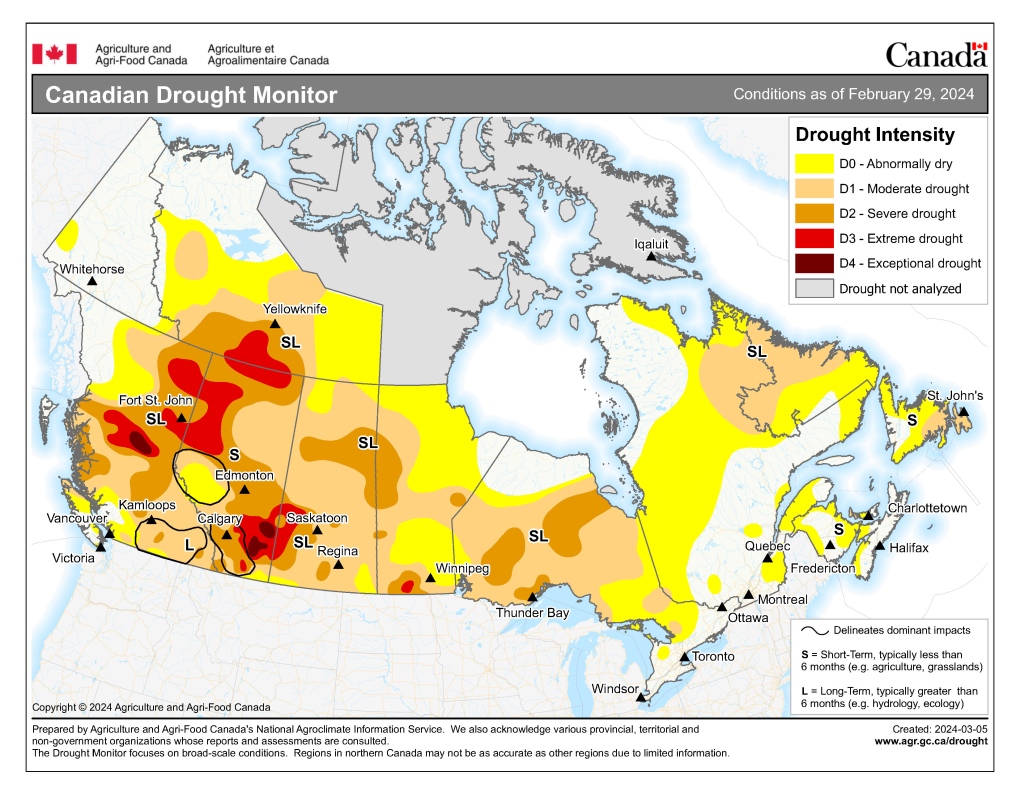 Drought conditions across Canada as of Feb. 29, 2024. (Agriculture and Agri-Food Canada)
Drought conditions across Canada as of Feb. 29, 2024. (Agriculture and Agri-Food Canada)
The government reports that 98 per cent of the Prairie region is currently classified as abnormally dry or in moderate to exceptional drought conditions.
Manitoba’s drought conditions are in line with what is being seen across the country. According to the report, February was one of the driest months for many regions around the country.
At the end of February, 71 per cent of Canada is classified as abnormally dry or in moderate to exceptional drought conditions. This includes 85 per cent of the country’s agricultural landscape.
View original article here Source




